Update: 26 April 2024
Health Screening, Medical Tests
Author: Julie Casper, C. Ac.
A search for "health screening harm" will retrieve about 9,700,000 results.
Health screening can be useful in clinical pathology. However, because of toxicity or the invasive nature of the procedure, some tests may do more harm than the condition that they are meant to identify.
Contents
- Understand the Trade-off Between Benefit and Harm
- Cancer Screening Harm
- Ovarian Cancer Screening and Mammograms
- Find objective information about any screening procedure you are considering.
- hTMA Screen - Comprehensive, Safe and Effective
- Health Screening References
- Resources
Understand the Trade-off Between Benefit and Harm1
Health screening is defined as the use of a test or a series of tests to detect unrecognized health risks or preclinical disease in apparently healthy populations to permit prevention and timely intervention. A health screening strategy consists of the sequence of a screening test, confirmatory test(s), and finally, treatment(s) for the condition detected.
The promised benefits of various health screenings are well publicized. The potential for physical and psychological harm is far less publicized. So it is up to you to decide. Here are some criteria to consider, a screening should be recommended only when these criteria are satisfied:
- The burden of illness should be high.
- The tests for screening and confirmation should be accurate.
- Early treatment (or prevention) must be more effective than late treatment.
- The test(s) and treatment(s) must be safe.
- The cost of the screening strategy must be commensurate with potential benefit.
"Many clinical communities now endorse widespread population screening to prevent the occurrence of cancer and cardiovascular disease. Breast cancer screening for women as young as 40, colon cancer screening for entire populations, and treatment to improve lipid profiles, even in very low risk patients are now widely advocated.
Many clinicians are unaware that to prolong a single life, hundreds of individuals must be screened for breast or colon cancer or treated with lipid profile-modifying agents for periods of up to a decade. The costs include anxiety as a result of the many false positive results, complications of invasive procedures such as lumpectomy or colonoscopy, side effects of treatment (including deaths as a result of a lipidlowering agent now withdrawn from the market) and resource investment that, at least for some individuals, might be better allocated elsewhere.
Clinicians should be aware there are important trade-offs in these decisions. If clinicians don't know the difference between an observational study and a randomized trial, or between a relative risk reduction and a risk difference, they are in no position to understand these trade-offs. If they are unable to understand the trade-offs, it is not possible for them to convey the possible benefits and risks to their patients, many of whom may, with a full understanding, decline screening or treatment."2
Gordon Guyatt, MD, McMaster University Medical College, Ontario, CanadaCancer Screening Harm
New research finds: In Australia alone, about 11,000 cancers in women and 18,000 in men may be overdiagnosed each year.
- Estimating the Magnitude of Cancer Overdiagnosis in Australia Study authors: Paul P Glasziou, Mark A Jones, Thanya Pathirana, Alexandra L Barratt and Katy JL Bell — Med J Aust. doi: 10.5694/mja2.50455
Can cancer screening do more harm than good? While most people believe that the earlier cancer is detected, the easier it will be to treat and cure, this common wisdom may not always be true. Some cancers may not be curable despite early detection, while other types of cancer may not have needed therapy in the first place.3
Dr. H. Gilbert Welch, is a professor at the The Geisel School of Medicine at Dartmouth and co-director of the V.A. Outcomes Group in the Department of Veterans Affairs in White River Junction, Vt. In a carefully researched, controversial book entitled, Should I Be Tested for Cancer? Maybe Not and Here's Why, Dr. Welch clearly explains why cancer testing can be a double-edged sword.
Tests like the PSA are forcing doctors and patients to think about the word "cancer" in a radically different way. Most of us think of it as a deadly disease if left untreated. But there are also microscopic cancers that will never cause problems. We all have abnormal cells, but most of us will not die from cancer. Pseudodisease is most common in prostate and breast cancer. But it is also an issue for kidney cancer, thyroid cancer, melanoma and lung cancer. When we look for cancer early, we cast such a wide net that we catch both real and pseudodisease. But we can't tell which is which, so we treat it all. And for many, treatment can only hurt. Dr. H. Gilbert WelchBack to Top
1.3 Million women received unnecessary, invasive cancer treatment.
"Breast cancer was over diagnosed. Tumors were detected that would never have led to symptoms in at least 1.3 million US women in the past 30 years." Gilbert Welch, Dartmouth Medical School
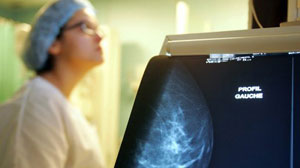
Routine mammograms have caused more than a million U.S. women to receive "unnecessary and invasive cancer treatments over the last 30 years," detecting tumors that are harmless. The results come after the government's Preventive Task Force issued recommendations in 2009 advising primary care physicians against recommending mammograms to women under 40 years of age.
Ovarian Cancer Screening and Mammograms
Tests commonly recommended to screen healthy women for ovarian cancer do more harm than good and should not be performed, according a panel of medical experts, the United States Preventive Services Task Force. Ovarian cancer screenings are blood tests for a substance linked to cancer and ultrasound scans to examine the ovaries. These tests do not lower the death rate from the disease, and they yield many false-positive results that lead to unnecessary operations with high complication rates.4
These recommendations are just the latest in a series of challenges to conventional cancer screenings that have been issued by this panel. They also reject P.S.A. screening for prostate cancer in men and routine mammograms in women under 50. The task force is a group of 16 experts, appointed by the government but independent, that makes recommendations about screening tests and other efforts to prevent disease. Its advice is based on medical evidence, not cost.
Back to TopFind objective information about any screening procedure you are considering.
If you simply ‘ask your doctor’ about the risks associated with a screening procedure, you may not get the complete picture.5 Try to find information about the screening from an objective source, one that does not profit from the procedure. In the United States we are guilty of using, and overusing, medical technologies.

What brings the pharmaceutical industry, some corporations, and even your local public health authorities together to offer "free" health screenings? Risks and dangers of free health screening
Some common health screening procedures may do more harm than good. Let's look at scans for example. For a PET scan, they inject radioactive glucose into your bloodstream, PET scans expose you to significant amounts ionizing radiation (a know carcinogen), newer procedures even combining PET with CT sans. CT scans and MRI scans utilize microwave radiation. Proponents of CT and MRI technologies suggest this type of radiation exposure is preferable to x-ray scans. Unfortunately, this claim is not supported by the scientific evidence. In fact, we do not know what the health consequences are of a wide range of man made electromagnetic radiation frequencies that have been introduced into the electromagnetic spectrum in recent decades. Unhappily, we are the experiment. We are bombarded with EMFs from cell phones and towers, satellite radio and TV transmission, "smart" meters, even the scanners at the airport.6 8

There are many other types of health screening procedures that can be detrimental to health.8 Colonoscopies, biopsies, mammograms, ultrasound, and whole body scans among them. And we haven't even mentioned the associated financial costs.
Diagnostic sonography (ultrasonography) is an ultrasound-based diagnostic imaging technique used for visualizing subcutaneous body structures including tendons, muscles, joints, vessels and internal organs for possible pathology or lesions. Obstetric sonography is commonly used during pregnancy and is widely recognized by the public. In physics, the term "ultrasound" applies to all sound waves with a frequency above the audible range of normal human hearing, about 20 kHz. The frequencies used in diagnostic ultrasound are typically between 2 and 18 MHz. Ultrasound has been shown to cause harmful effects in body tissues and abnormalities in embryos and offspring of animals and humans. A blast of ultrasound over the testicles can make a man infertile for six months. And they are actually considering using this treatment for male contraception. One can't help but wonder what ultrasound during pregnancy is doing to the fertility potential of male fetuses. A study performed in Sweden in 20019 has shown that subtle effects of neurological damage linked to ultrasound were implicated by an increased incidence in left-handedness in boys (a marker for brain problems when not hereditary) and speech delays.10 11
50 Human in utero studies indicate extreme risk for prenatal ultrasound

Author Jim West includes over 50 studies of in utero fetal exposure to prenatal ultrasound. The conclusions are stunning, with recommendations that ultrasound should be completely avoided "for a quality pregnancy." The studies, done in China, provide empirical evidence of ultrasound hazards. Previously, it was assumed humans were resistant to ultrasound toxicity.
From a medical standpoint, ultrasonic fetal scanning is generally considered safe and is properly used when medical information on a pregnancy is needed. But ultrasound energy delivered to the fetus cannot be regarded as completely innocuous. Laboratory studies have shown that diagnostic levels of ultrasound can produce physical effects in tissue, such as mechanical vibrations and rise in temperature. Although there is no evidence that these physical effects can harm the fetus, public health experts, clinicians and industry agree that casual exposure to ultrasound, especially during pregnancy, should be avoided. Viewed in this light, exposing the fetus to ultrasound with no anticipation of medical benefit is not justified. Persons who promote, sell or lease ultrasound equipment for making "keepsake" fetal videos should know that the FDA views this as an unapproved use of a medical device. There is a wide difference in the training and skill of the sonographer or sonologists, and in the quality of the equipment used. Improvements in equipment sensitivity has lead to the earlier detection of abnormal structures in the fetus, causing false-positive diagnoses that could generate undue anxiety in patients.
Back to TopDental Screening Risks
Even the routine screenings you receive from a dentist should be reevaluated. When possible, resist x-rays unless absolutely necessary. For one thing, x-rays are very difficult to interpret correctly, even for an expert radiologist. The cancer causing effects of ionizing radiation from an x-ray are well documented in the scientific literature. In addition, the definitive dental information that an x-ray is able to show is very limited. For example, it is impossible to demonstrate infection with an x-ray because dental radiographs show hard tissue only. They do not accurately represent soft tissue, or infections. Due to the shadow cast by the root it also may be impossible to see bone loss. Dentists are taught that a root canal must be filled to within 1mm of the root apex. The apex of a root canal is only rarely determinable by x-ray. Thus many root canals are worked too short, or too long so that the root filling will protrude through the end of the tooth and into the bone. This is well documented research published in conventional dental literature (e.g., "In the canals which were overfilled, the extruded materials were always associated with advanced destruction of the surrounding tissue and liquefaction necrosis" Malcolm Davis - Periapical and intracanal healing following incomplete root canal fillings in dogs, Oral Surgery, May 1971, Vol. 31 No. 5)
Conventional dentistry is riddled with toxicity, root canal therapy, mercury amalgam fillings, fluoride, and more. Dental health is essential to overall health.
Back to TophTMA Screen - Comprehensive, Safe and Effective
Hair analysis as a nutritional screening tool.
By David L. Watts, Ph.D., Director of Research, ©Trace Elements, Inc.
Hair is an ideal tissue for nutritional and toxic metal assessment for several reasons. Taking a hair sample is non-invasive, easily collected, stored and transported. All of the important nutritional elements and toxic elements accumulate in the hair. It has been found to be especially suitable for biological monitoring of environmental exposure on a global, regional, and local level. Nutritional assessment using hair mineral analysis has many advantages compared to mineral analysis of other tissues in that it shows retention of minerals by the body. Testing metals in the urine only measures the minerals that are being excreted. The blood gives an indication of the minerals that are absorbed and temporarily in circulation before they are excreted and/or sequestered into storage depots. Blood and urine testing gives an indication of the mineral status of the body only at a specific time. However, mineral concentrations found in the hair represents long-term intake or exposure making it more useful for nutritional and epidemiological studies.
Today, individual nutritional deficiencies such as scurvy and beri beri are rare. However, undernutrition and nutritional imbalances are a major problem. As an example, calcium and magnesium work together for many functions within the body. Magnesium alone is responsible for the function of hundreds of enzymes. However, normal enzyme activity can be disturbed not only by a deficiency of magnesium but also when the normal relationship between calcium and magnesium is lost. A person can have adequate amounts of magnesium, but if their calcium is too high, a relative magnesium deficiency exists that can contribute to abnormal function and ultimately adverse health conditions. Not only can individual deficiencies and excesses be seen in a hair mineral analysis, but also the many interrelationships between elements can be viewed and interpreted through a single sample. At present, hair mineral analysis is the most economical and useful screening tool for evaluating nutritional interrelationships in individuals as well as population groups. Follow-up tests also aid in assessing improvements in nutritional status following supplementation, dietary and lifestyle changes.
How vitamin needs can be evaluated thorough hair analysis tests.
Minerals interact not only with each other but also with vitamins, proteins, carbohydrates and fats. Minerals influence each of these factors, and they, in turn, influence mineral status. Minerals act as enzyme activators, and vitamins are synergistic to minerals as coenzymes. Therefore, it is extremely rare that a mineral disturbance could develop without a corresponding disturbance in the synergistic vitamin(s). By the same token, it would be rare for a disturbance in the utilization or activity of a vitamin to occur without a synergistic mineral(s) also being affected. Vitamin D depletion, for example, can be assessed by measurement of its function. Vitamin D is closely related to the minerals calcium, magnesium and phosphorus. A number of syndromes result from vitamin D deficiency, all related to a deficiency or imbalance between the minerals calcium, phosphorus and magnesium. Vitamin C affects iron absorption and reduces copper retention. Boron and iron influence the status of vitamin B2. Vitamin B2 affects the relationship between calcium and magnesium. Vitamin B1 enhances sodium retention, B12 enhances iron and cobalt absorption, and vitamin A enhances the utilization of zinc and yet antagonizes vitamin D and E. Protein intake will affect zinc status, etc. Therefore, evaluating one's mineral status gives good clues to one's vitamin status and requirements. Research at TEl involves recognizing the many synergistic and antagonistic interrelationships between minerals and vitamins.
Differences between hair mineral levels and blood mineral levels.
Minerals circulating in the blood are under a very different homeostatic control than minerals in the tissues. They must be maintained within narrow limits in the blood. This is accomplished even if the dietary intake of a nutrient is very high or very low. Maintaining minerals within a range in the blood is attained several ways. If a mineral intake is very high, the body will compensate by removing or eliminating it as quickly as possible. If the mineral is not eliminated, it will be stored in body tissues. If intake of an element is very low, then the body will draw from storage areas to maintain blood levels. Once the storage level of a mineral is markedly depleted, then the blood will reflect a deficiency. Other factors affect blood mineral levels such as stress, inflammation, other disease states, and medications. Therefore, blood mineral levels will not always correlate with tissue mineral status since blood mineral levels are usually maintained at the tissue's expense.
Acceptance of hTMA for screening.
Hair mineral tests have long been accepted as a routine test for toxic metal screening and investigations of environmental contamination and disease. It has been used extensively for nutritional studies in humans and animals. For over 30 years nutritionists, dietitians, and doctors who are concerned about their patients' nutritional status and who are aware of the vast amount of research showing the relationship of nutrition to disease incorporate hair mineral analysis in their practice as a routine evaluation and screening tool. When a hair sample is properly obtained, analyzed and interpreted, it has proven to be an economical screening tool for toxic metal exposure as well as a good indicator of nutrient interrelationships and nutritional status.
hTMA References
- Trace Elements and Other Essential Nutrients. Watts, D.L. T.E.I., 1995.
- Hair, Trace Elements, and Human Illness. Eds. Brown, A.C., Crounse, R.G. Praeger Pub.1980.
- Hair Analysis. Applications in the Biomedical and Environmental Sciences. Chatt, A., Katz, S.S. VCH Pub. 1988.
- Human Hair Vol. 1. Fundamentals and Methods for Measurement of Elements Composition. Valkovic, V. CRC Press. 1988.
- Human Hair, Vol II. Trace-Element Levels. Valkovic, V. CRC Press. 1988.
- Laboratory Tests For The Assessment Of Nutritional Status. Sauberlich, H.E., et al. CRC Press. 1984.
- Trace Substances in Environmental Health. Ed. Hemphill, D.D. Univ. Mo. Columbia. 1972-1986.
- Analysis of Zinc levels In Hair for the Diagnosis of Zinc Deficiency in Man. Strain, W.H., et. al. J. Lab. Clin. Med., 1966.
- Determination of Aluminum, Copper, and Zinc in Human Hair. Stevens, B.J. Atomic Spectroscopy. 1983.
- The use of Hair as a Biopsy Material for Trace Elements in the Body. Katz, S.A. Am. Lab. 1979.
- Hair Trace Element Levels and Environmental Exposure. Hammer, D.l., et. Al. Am. J. Epid. 1971.
- Hair Chromium Concentration of Human Newborn and Changes During Infancy. Hambridge, K.M., Baum, J.D. Am. J. Clin. Nutr. 1972.
- Trace Element Nutriture and Metabolism Through Head Hair Analysis. Strain, W.H., et al. Trace Substances in Environmental Health. Ed. Hemphill, D.D. Univ. Mo., Columbia. 1974.
- Lead in Hair in Children with Chronic Lead Poisoning. Kopito, L., et al. New Eng. J. Med. 1967.
- Chronic Plumbism in Children: Diagnosed by Hair Analysis. Kopito, L., et al. J. Am. Med. Assoc. 1968.
- Magnesium Content of Hair in Alopecia Areata Atopica. Cotton, D., et al. Dermatologica. 1976.
- Hair Manganese Concentrations in Newborns and Their Mothers. Saner, G., et al. Am. J. Clin. Nutr. 1985.
- Elevated Hair Copper Levels in Idiopathic Scoliosis. Pratt, W., Phippen, W. Spine. 1980.
- Low levels of Zinc in Hair, Anorexia, Poor Growth, and Hypogeusia in Children. Hambridge, K.M., et a!. Peadiatr. Res. 1972.
- Hair Minera.l Levels and their Correlation with Abnormal Glucose Tolerance. Tamari, G.M., Rona, Z. Cytobiological Rev. 1985.
- Hair and Urine Chromium Content in 30 Hospitalized Female Psychogeriatric Patients and Mentally Healthy Controls. Vobecky, J., et al. Nur. Rep. Inti. 1980.
- Hair as an Indicator of Excessive Aluminum Exposure. Yokel, R.A. Clin. Chem. 1982.
- Comparison of Concentrations of Some Trace, Bulk and Toxic Metals in the Hair of Normal and Dyslexic Children. Capel, I.D., et al. Clin. Chem. 1981.
- Hair Zinc Concentrations in Diabetic Children. Amodor, M., et al. Lancet. 1975.
- Blood pressure in Young Adults as Associated with Dietary Habits, Body Conformation, and Hair Element Concentrations. Medeiros, D.M., et al. Nutr. Res. 1982.
- Sodium, Potassium, Calcium and Magnesium in Hair from Neonates with Cystic Fibrosis and in Amniotic Fluid from Mothers of such Children. Kopito, L., et al. Pediatrics. 1972.
- Cadmium, Copper, Lead, Mercury, and Zinc Concentrations in the Hair of Individuals Living in the United States. Interface. 1973.
- Hair Analysis for the Observation of Magnesium Deficiency or Excess. Strain, W. Magnesium in Health and Disease. Spectrum Pub. 1980.
- Trace Elements in Scalp-Hair of Persons with Multiple Sclerosis. Ryann, D., et al. Clin. Chem. 1980.
- Concentration of Chromium in the Hair of Normal Children and Children with juvenile Diabetes Mellitus. Hambridge, K.M., et al. Diabetes. 1968.
- Interrelationships of Blood and Hair Mercury Concentrations in a North American Population Exposed to Methylmercury. Phelps, R. W. , et al. Arch. Environ. Hlth. 1980.
- Measurement of Mercury in Human Hair. Giovanoli-Jakubczak, T., et al. Arch. Environ. Hlth. 1974.
- On Nickel Contents in Urine and Hair in a Case of Exposure to Nickel Carbonyl. Hagedom-Gotz, H. et al. Arch. Tox. 1977.
- Hair Chromium Concentration and Arteriosclerotic Heart Disease. Cote. M., et al. Chromium in Nutrition and Metabolism. Eds. Shapcott, D., Hubert, J. Elservier Press. 1979.
- Arsenic Concentration in Drinking Water, Hair, Nails, Urine, Skin-Scale and Liver Tissue of Affected People. Chatergee, D.D., et al. Analyst. 1995.
- Arsenic Levels in Hair of Workers in a Semiconductor Facility. De Peyster, A., et al. Am. Ind. Hyg. Assoc. Vol. 56. 1995.
- Studies on the Concentrations of Arsenic, Selenium, Copper, Zinc and Iron in the Hair of Blackfoot Disease Patients in Different Clinical Stages. Wang, C.T., et al. Eur. J. Clin. Biochem. 1994.
- Beard Calcium Concentration as a Marker for Coronary Heart Disease as Affected by Supplementation with Micronutrients including Selenium. MacPherson, A., et al. Analyst. 1995.
- Hair Chromium Content of Women with Gestational Diabetes Compared with Nondiabetic Women. Aharoni, A., , et al. Am. J. Clin. Nutr. 1992.
- Cadmium, Copper, Lead and Zinc Concentrations in Human Scalp and Pubic Hair. Wilhelm, M., et al. Sci. Tot. Environ. 1990.
- Lithium in Scalp Hair of Adults, Students, and Violent Criminals. Effects of Supplementation and Evidence for Interactions of Lithium with Vitamin B12 and with Other Trace Elements. Schrauzer, G.G., et al. Biol. Trace Elem. Res. 1992.
- Concentration of Magnesium in Hair of Inhabitants of Down-Town Krakow, The Protective Zone of Steel-Mill "Hutaim Sendzimira" and Tokarania Village. Solarska, K., et al. Przel Lek. 1995.
- Iron, Copper, Cadmium, Zinc and Magnesium Contents of Urinary Tract Stones and Hair From Men with Stone Disease. Durak, I., et al. Euro. Urol. 1990.
- Effects of Long-Term Anticonvulsants Therapy on Copper, Zinc, and Magnesium in Hair and Serum of Epileptics. Suzuki, T., et al. J. Bioi. Psychiatry. 1992.
- Metals in Hair as Biological Indices for Exposure. Foo, S.C., et al. Int. Arch. Occup. Environ. Hlth. 1993.
- Mercury Levels in Hair from People Eating Large Quantities of Swedish Freshwater Fish. Okarsson, A., et al. Food Addit. Contam. 1990.
- Use of Hair Analysis for Evaluating Mercury Intoxication of the Human Body. Katz, S.A., Katz, R.B. J. Appl. Toxicol. 1992.
- Nickel in Nails, Hair and Plasma from Nickel-Hypersensitive Women. Gammelgaard, B., et al. Acta. Derm. Venereol. 1990.
- Platinum in the Human Diet, Blood, Hair and Excreta. Vaughan, G.T., Florence, T.M. Sci. Tot. Environ. 1992.
- Determination of Hair Trace Elements in Childhood Celiac Disease and in Cystic Fibrosis. Varkonyi, A., et al. Acta. Ped. 1992.
- Study of Correlation of Selenium Content in Human Hair and Internal Organs by INAA. Cheng, Y.D., et al. Bioi. Trace Elem. Res. 1990.
- Emission Spectrophotometric Analysis of Titanium, Aluminum, and Vanadium Levels in the Blood, Urine, and Hair of Patients with Total Hip Replacement. Trinchi, V., et al. J. Orthop. Traumatol. 1992.
- Hair Zinc and Copper Concentrations and Zinc: Copper Ratios in Pediatric Malignancies and Healthy Children from Southeastern Turkey. Donma, M.M., et al. Bioi. Trace Elem.Res. 1993
- Hair Zinc and Dietary Zinc Intake During Pregnancy and Puerperium. Carbone, P., et al. J. Obstet. Gyn. Reprod. Biol. 1992.
- Relationship Between Zinc in Serum and Hair and some Hormones During Sexual Maturation in Humans. Vivoli, G., et al. Sci. Tot. Environ. 1990.
- Trace Elements Nutritional Status. Use of Hair as a Diagnostic Tool. Contiero, E., Folin, M. Biol. Trace Elem. Res. 1994.
- Trace Elements in the Hair of Healthy and Malnourished Children. Weber, C.W., et al. J. Trop. Pediatr. 1990.
- Study on the Relation of Selenium, Manganese, Iron, Strontium, Lead, Zinc, Copper, and Calcium to Liver Cancer Mortality from Analysis of Scalp Hair. Wang, Y.X., et al. Sci. Tot. Environ. 1990.
- Trace Elements in Hair as Related to Exposure in Metropolitan New York. Creason, J.P., et al. Clin. Chem. 1975.
- Analysis Of Copper And Lead In Hair Using The Nuclear Microscope; Results From Normal Subjects, and Patients With Wilson's Disease and Lead Poisoning. Watt, F., et al. Analyst Vol.120, 1995.
- Hair Iron Content: Possible Marker to Complement Monitoring Therapy of Iron Deficiency in Patients with Chronic Inflammatory Bowel Disease. Bisse, E., et al: Clin. Chem. Vol.42, 1996.
- Monitoring of Cadmium, Copper, and Lead and Zinc Status in Young Children Using toenail: Comparison with Scalp Hair. Wilhelm, M., et al: Sci. Tot. Environ. Vol. 103, 1991.
- Traceelements in Full-Term Neonate Hair. Moro, R. et al: J. TraceElem. Electrolytes Health Dis. Vo1. 6, 1992.
- Coronary Atherosclerosis and Chemical Traceelements in the Hair. A Canonical Correlation Study of Autopsy Subjects, Using and Atheromelric System and the X-ray Flurorescence Analysis. Fernandez-Britto, J.E., et al: Zentralbl Pathol. Vol. 139, 1993.
- Hair Analysis of Spastic Children in Hong Kong. Man, C.K., et al: Sci. Tot. Environ. Vol. 191, 1996.
- Age-Related Decreases in Chromium Levels in 51,665 Hair, Sweat, and Serum Samples from 40,872 Patients - Implications for the Prevention of Cardiovascular Disease and Type II Diabetes Mellitus. Davies, S., et al: Metabolism. Vol. 46, 1997.
- Impact of Reduction of Lead in Gasoline on the Blood and Hair Lead Levels in the Population of Tarragona Province, Spain, 1990-1995. Schuhmacher, M., et al: Sci. Tot. Environ. Vol. 184, 1996.
- Hair Lead Levels Related to Children's Classroom Attention-Deficit Behavior. Tuthill, R.W. Arch. Environ. Health. Vol. 51, 1996.
Health Screening References
- Trade-off between benefit and harm is crucial in health screening recommendations. Part I: General Principles. National Center for Biotechnology Information, U.S. National Library of Medicine
- Painless evidence-based medicine / edited by Antonio L. Dans, Leonila F. Dans, Maria Asuncion A. Silvestre; foreword by Gordon Guyatt. [DNLM: 1. Evidence-Based Medicine. WB 102 P147 2007]
- Can Cancer Screening Do More Harm Than Good? Dartmouth-Hitchcock Cancer Center
- Research: Ovarian Cancer Screenings Are Not Effective U.S. Preventive Services Task Force
- Death by Health Screening: The Risks and Dangers of Free Health Screening Health Alert
- Electromagnetic Fields: A consumers guide B. Blake Levitt
- Resonance - Beings of Frequency documentary film (1 hr 28 min)
- Dial back esophageal cancer screening: internists Reuters Health
- Kieler, H; Cnattingius, S; Haglund, B; Palmgren, J; Axelsson, O (2001). "Sinistrality—a side-effect of prenatal sonography: A comparative study of young men." Epidemiology (Cambridge, Mass.) 12 (6): 618–23. doi:10.1097/00001648-200111000-00007. PMID 11679787.
- Salvesen, K.; Vatten, L. J.; Eik-Nes, S. H.; Hugdahl, K.; Bakketeig, L. S. (1993). "Routine ultrasonography in utero and subsequent handedness and neurological development." BMJ: British Medical Journal 307 (6897): 159–164. doi:10.1136/bmj.307.6897.159. JSTOR 29720401. PMC 1678377. PMID 7688253.
- Kieler, Helle; Axelsson, Ove; Haglund, Bengt; Nilsson, Staffan; Salvesen, Kjell Å. (1998). "Routine ultrasound screening in pregnancy and children's subsequent handedness." Early Human Development 50 (2): 233–45. doi:10.1016/S0378-3782(97)00097-2. PMID 9483394.
Resources
- Private health screening tests are oversold and underexplained Margaret McCartney
- Lies, Damned Lies, and Medical Science By David H. Freedman
- Choosing Wisely Imaging tests for lower-back pain usually do not help.
- Blinded by Science (introduction) by Matthew Silverstone
- Should You Run from that Medical Test?
- Seeking Sickness Medical Screening and the Misguided Hunt for Disease.
- Excessive Medical Spending - Facing the challenge By Norman Temple, Andrew Thompson
- Selling Sickness with Alan Cassels (24 min) Pacifik Media
- Routine ultrasound testing not proven safe for pregnant women Dr. Megan Heimer J.D, N.D.